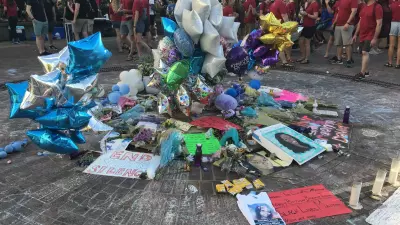Three years ago, the former Bellevue General Hospital stood practically empty — a building with more than a century of rich history but no real future.

Now efforts to make the former 154-bed hospital a community hub in Bellevue, Pa., are once more gaining momentum. The hope, leaders say, is to provide a new approach to shuttered hospitals, a result of financial hardships afflicting many similarly situated communities across Postindustrial America.
Among other factors, dwindling population centers leave behind people who are more chronically ill and, often, more reliant on Medicare and Medicaid. Those programs reimburse hospitals at significantly less than the cost of care — and even when patients have commercial insurance, those health plans typically reimburse rural hospitals at a lower rate than they do for urban facilities. Add those strains to an ongoing health-care labor shortage, and the result is a bottom line that many hospital associations and policy analysts say will flatline without outside intervention.
It’s a scenario that plays out across communities like Bellevue, where core industries have disappeared, according to Allegheny Health Network Chief Physician Executive of Community Health and Innovation Dr. Jeff Cohen.
“This was an upper middle-class community until steel died,” Cohen said.
Like communities across the region, Bellevue, just outside of Pittsburgh, has experienced population loss — about 28% since 1970, to 8,100. The hospital’s emergency department closed in 2010, and a portion of the 230,000-square-foot building served as a skilled nursing facility until June 2019.
Cohen was president of Allegheny General Hospital from 2016 to 2019. Now, he and the leadership team at the Bellevue facility — AHN Suburban — are on a mission to resurrect the space and reinvigorate the community through a “community health” approach.
The concept, initiated in 2020, was to build out a health-care technology accelerator, rent administrative spaces for companies, and make room for nonprofits and community initiatives.
The building now houses: a tech accelerator space with offices and labs for biotechnology, pharmaceutical, and biomedical startups; after-school programming and STEM opportunities for local students; former patient rooms that have been converted into office spaces, including three international headquarters for private companies; a nonprofit organization that offers minority-owned culinary businesses access to the 6,000-square-foot commercial kitchen.
There are also nonprofits based there that are working to address housing inequality, food insecurity, workforce development gaps, and other needs in the region.
“We phrase this as community health, not health care,” Cohen said. “The economics directly correlate with it, so this facility should be geared toward dealing with social factors.”
Today, there are now about 30 organizations making use of the building. That’s in addition to AlphaLab Health, the 10,000-square-foot life-sciences accelerator launched in 2020 in partnership with nonprofit business incubator Innovation Works.

The accelerator program is now on track to graduate a third six-company cohort this spring.
AHN has invested $1.8 million in the startups so far, with more than $20 million in follow-on investments made in those new companies.
The other numbers seem to be working out too.
With a formal opening this February for new primary and express care services on the building’s ground floor and a recently opened exercise-oncology gym for cancer patients, administrators already have filled about 65% of rentable space in the building overall.
The hospital also has served as a filming location for movies and TV shows — another unconventional idea that has helped improve the financial picture.
While Stephen Hunter, AHN’s vice president of innovation and incubator operations, said his measurements of success include numbers like meals created and students supported, the facility has also achieved financial solvency. Its rental income covers maintenance and operating costs.
And the unique, multifaceted model appears to be gaining momentum, he said.
“Many closed hospitals are repurposed into other clinical assets — a medical mall or assisted living facility,” Hunter said. “Some ultimately just become nothing. Some are in prime real estate and will probably become something new. Hahnemann Hospital in Philadelphia is downtown and could become a hotel or retail.
It’s not an approach that’s widespread; in some other areas new development is replacing old hospitals, instead of repurposing the facilities.
Other endeavors incorporate some elements of the concepts at work in Bellevue.
Inception Health — owned by Milwaukee-based Froedtert and the Medical College of Wisconsin — launched eight years ago to develop health-care innovation and digital tools in a 10,000-square-foot office space previously used for outpatient ambulatory services in Froedtert Hospital’s North Hills Health Center in Menomonee Falls, Wis.
The Jump Simulation & Education Center at Peoria, Ill., represents a collaboration between OSF HealthCare and the University of Illinois College of Medicine Peoria and offers a full operating theater and other simulation spaces for testing new technologies, but those spaces were all constructed as part of a $55 million renovation — rather than being repurposed from existing hospital facilities.
Some health systems have replaced a closed general hospital with new or repurposed clinical facilities and some social programming, Cohen said, but the hope is that the former AHN hospital can become an example of how much those sprawling hospital spaces still have to offer — in a much broader sense.
“Can we afford to have health care go through what steel went through? The short answer is ‘no.’ So how do you get in front of it?” Cohen said. “How do you repurpose a hospital? The hospital is the geographic center for health care through the 20th century, but it’s built on a manufacturing model. Now we’ve got to find answers for the 21st century.”
Rural hospitals’ ongoing crisis
Across the country, communities are searching for those answers, often amidst a struggle to survive, particularly in rural areas.
In a quarterly report by the Center for Healthcare Quality and Payment Reform, hospitals located in communities that the federal government defines as “rural” are evaluated for risk of closure.
The report released this January identifies 631 hospitals that are considered “at-risk” due to a combination of financial losses in delivering patient services and low financial reserves.
Pennsylvania has 12 rural hospitals on that list — 30% of the total number of rural hospitals statewide. New York, Tennessee, and Georgia all have 21. Alabama’s 29 at-risk rural hospitals included in the report account for 60% of the state’s total rural hospitals.
In the center’s quarterly evaluations, patient service losses are a core piece of the puzzle, according to Harold Miller, the center’s president and adjunct professor of public policy and management at Carnegie Mellon University.

“Fundamentally, a hospital is always going to have a problem if it can’t actually make money delivering the services patients need,” he said. “Relying on local taxes or subsidies to offset losses is potentially problematic or unsustainable. If a commercial plan is paying less than the cost, that needs to be fixed. Ideally, small hospitals should receive a standby capacity payment to ensure they can sustain essential services.”
As for the impact of closures, that varies by community.
In places like Bellevue, where there are other nearby health-care options, a closure has a different effect than places where access is more complex, Miller said.
That impact is, of course, magnified even more in an isolated town in Mississippi or a frontier community in a more sparsely populated state, he added.
“Many of these small rural hospitals are literally the only health care in the community,” he said. “There is no urgent care center. There is no primary care physician. When the hospital closes, the community has lost everything. Some of these small rural hospitals are also the community’s nursing home. When those hospitals close, all of that is gone.”
REPORT: WHAT HAPPENED TO MY HOSPITAL?
Why small-town hospitals are closing in record numbers — and what can be done
Hospitals in rural areas are closing in record numbers, and the problems are expected to worsen.
That’s according to a 2022 report by the American Hospital Association. The report examined the factors behind a decade of rural hospital closures —136 from 2010 to 2021— and raised concern that these pain points will persist, as they did with a record 19 closures in 2020.
Shannon Wu, the association’s senior associate director of payment policy, said that the temporary, federal emergency assistance that offered a reprieve in 2021 won’t be enough to shift course. This year, the Department of Health and Human Services announced plans to end the public health emergency for COVID-19 in May 2023, which likely spells the end of pandemic-related federal assistance for hospitals.
“Unfortunately, we don’t expect the trend we saw in the report to change,” Wu said. “We expect that these rural hospital closures will continue to increase.”
One foundational problem is that declining populations in rural areas mean less money available to cover fixed operating costs.
Two more challenges add pressure to many rural hospitals’ existential crisis, Wu said: Medicare and Medicaid don’t reimburse at a rate that covers the cost of care. On top of that, there are ongoing staffing shortages.
Recruiting and retaining healthcare professionals in rural communities remains challenging, she said. Doctors and nurses often prefer working in areas that command better salaries, and closer to large cities.
“Rural hospitals and rural providers overall have traditionally faced significant staffing shortages across the board and across time as well,” Wu said.
About 10 percent of physicians practice in rural communities even though 20 percent of the U.S. population lives there, she said.
“I think rural communities and rural providers feel that very acutely, and that issue was brought to light again during the pandemic,” Wu said.
The report also highlights the impact: Vulnerable groups — senior citizens, low-income individuals and those suffering chronic conditions — are disproportionately affected when hospitals in rural areas close.
These often are the same groups that lack transportation access, so traveling farther to a hospital is a potentially life-threatening barrier to care.
Wu said there’s no single solution, but policy changes may provide some relief.
One example is the new Rural Emergency Healthcare Model, launched in January.
“Medicare is allowing, for the first time, federal dollars to go to facilities that provide emergency care without the need to provide inpatient care,” she said. “We’re really looking to see and support unique payment models and innovative ideas.”
That move could help alleviate some of the fixed costs of keeping inpatient facilities open when the volume has diminished, she said, while still allowing hospitals to at least maintain an emergency department — a critical service.
Those Rural Emergency Healthcare providers could still offer other high-demand outpatient services like behavioral health or maternal health, or they could partner with nearby clinics to address a broader level of care.
The idea is to find ways to keep doors open.
Partnerships, mergers, and affiliations are increasing across the country, and sometimes those approaches present the most viable option, Wu said. While concerns remain that affiliations increase closures, a Hospital Association analysis of UNC Sheps Center rural hospital data shows that less than half of the hospitals that closed from 2010 to 2020 were system-affiliated.
“We support policies that allow flexibility for rural communities, hospitals, and providers,” Wu said. “For them to be able to explore different partnerships, whatever that relationship might be — an acquisition from another hospital, contracts around transfers of patients, or even a shared workforce that allows physicians to travel between different locations — we support the flexibility because we know every rural area and community is very different. And the question often comes down to whether they will have to close or not.”